We all know that the COVID-19 pandemic has had a huge impact on the wellbeing of staff.
Sometimes though, we don't allow ourselves to fully appreciate how tough things have been for us personally. There are very understandable reasons that you are finding things hard at the moment. Even if things at work have improved for the time being, the situation you were in over the last 18 months may well still be having an impact. What you have been through may have left you feeling depleted. On top of that, you may have concerns about what your work will be like in the coming months.
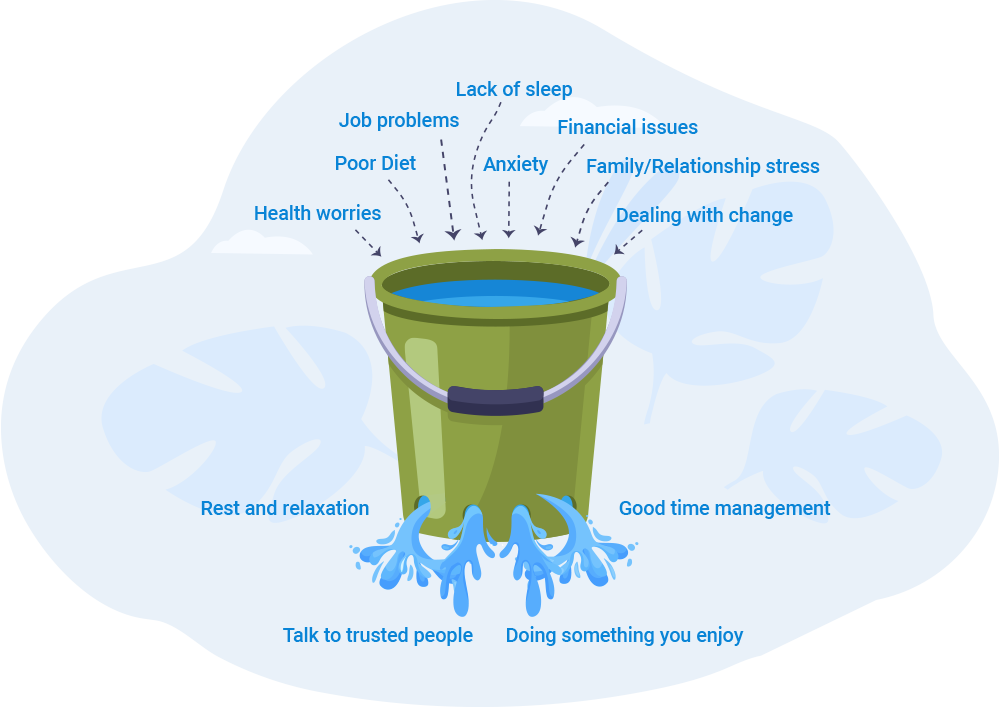
Here are just some of the many pressures that you may have been under in your own role. Have a think about which of these apply to you, or whether there are others which are not listed.
- Increased workload and working hours.
- Intensity of working in different / COVID-19-safe environment.
- The isolation of working from home.
- Guilt about shielding or working from home.
- The impact of the heroes' narrative including the clapping.
- Emotional strain from seeing large numbers of patients dying.
- Anxiety about your own and loved ones' health and infection risk.
- Worries about being able to provide high-quality care.
- Having to undertake new procedures with minimal training/support or work outside of your job role.
- Unfamiliar working conditions or unknown environments.
- Reduced staff ratios and skill mix, which may have increased other safety risks.
- Lack of standardisation across wards for equipment, layout, and bed numbering systems.
- Difficulty accessing PPE, and/ or the discomfort of wearing it for extended periods.
- Escalation pathways not known or provided, or staffed, or the designated person for escalation inexperienced in that area or that task.
- Rapidly changing guidance - for those who worked part time, procedures and guidance changed, often dramatically, during days off.
- The temporary loss of the things that used to reduce stress, e.g., not being able to socialise, or go to the gym.
- We are hearing from staff that they are fearful of an increase in COVID cases this winter. This fear hanging over staff is very draining;
We've all got that Covid fatigue. We're exhausted by the way we're living and working. And it's really difficult. The thing is, we're coming up to winter, we've got to step up to the mark again. And it's whether we have the resilience to deal with that. And, of course, we'll have to because there's just no more capacity and no more staff to handle it.
(Lead Cancer Nurse from Macmillan)
Written evidence submitted by Macmillan Cancer Support (WBR0053))
- Staff are especially concerned that there will be less efforts to redeploy staff into the most needed areas for another wave. Without these extra pairs of hands, frontline staff are worried about how they will cope with demands.
- Many are worried about how the non-emergency teams can even begin to tackle the waiting lists for procedures, operations, and tests.
If you experienced any of the above, you are not alone.
It's no surprise that many of us are finding that we don't feel ourselves at the moment, ranging from mild stress type symptoms to severe anxiety difficulties or depression. Studies show that this is the case:
- The Nursing Times suggested there had been a 37% increase in the number of mental health-related absences across the NHS from February to June 2021.
- In May 2020 over half of the members of the Royal College of Psychiatrists said that their wellbeing had worsened.
- The Nursing Times reported that 90% of respondents to a survey felt higher rates of anxiety than before the pandemic.
If any of this resonates with you, if you feel depleted from what has happened, or from your fears about what is yet to come, please see our pages about anxiety and low mood and the available support.